F2 Teaching Day (Aug)
This week we held the first F2 teaching day for our newest rotation of junior doctors at Leicester Royal Infirmary’s ED. We had a smörgåsbord of topics from mental health, through to minor injuries and managing head injuries.
Here's a summary of some of the key learning points from the day…
Mental Health
Primary Assessment
Physical health needs:
Observe the patient, look for any injuries or evidence of self-harm
Assess their cognition
Environment:
Is the environment safe for you?
Is the environment safe for the patient?
Personal possessions:
Does the patient have any potential weapons on them?
Remove anything that could be used to harm themselves
Intent:
Any thoughts to harm self or others
Any desire to leave
Assessment of Risk
Suicidal thoughts:
What were they thinking at time of episode?
Did they want to die?
Lethality of episode:
Would it have resulted in death?
Made efforts not to be found
Intent now:
Any current thoughts to self-harm
Do they have any regrets?
Protective or Adverse factors:
Aspects can be protective and/or adverse…
Jobs, relationships, friends and family
Criminal charges
Risk factors and past/current mental health problems.
Capacity
A person is presumed to have capacity and can refuse treatment…
Person must understand the information given to them
Retain the information
Weigh up the information to come to a decision
Communicate that decision
If refusing, explore why they are refusing and consequences of refusing.
Resources
- RCEM Learning: Psychiatric Emergencies for the Adult Patient (module)
- RCEM: Mental Health Toolkit
- Emergency Medicine Cases: Medical Clearance of the Psychiatric Patient (podcast)
Toxicology
Intentional and Non-Intentional overdoses are managed in the same way at the start.
Find out…
What was taken?
Consider activated charcoal if within 60 minutes
How much was taken?
When was it taken?
Was anything else taken with it? (e.g. alcohol or other drugs)
Check on Toxbase.org for investigations…
Bloods (FBC, U&E, LFT, CK, Clotting, VBG)
ECG (rate, rhythm, QTc)
Once treated get Mental Health assessment (if indicated)
Resources
- TOXBASE®
- Core EM: Toxicology-related articles
- RCEM Learning: Toxicology-related modules (#CAP27)
- Emergency Medicine Cases: Salicylate Poisoning & Low and Slow Poisoning (podcasts)
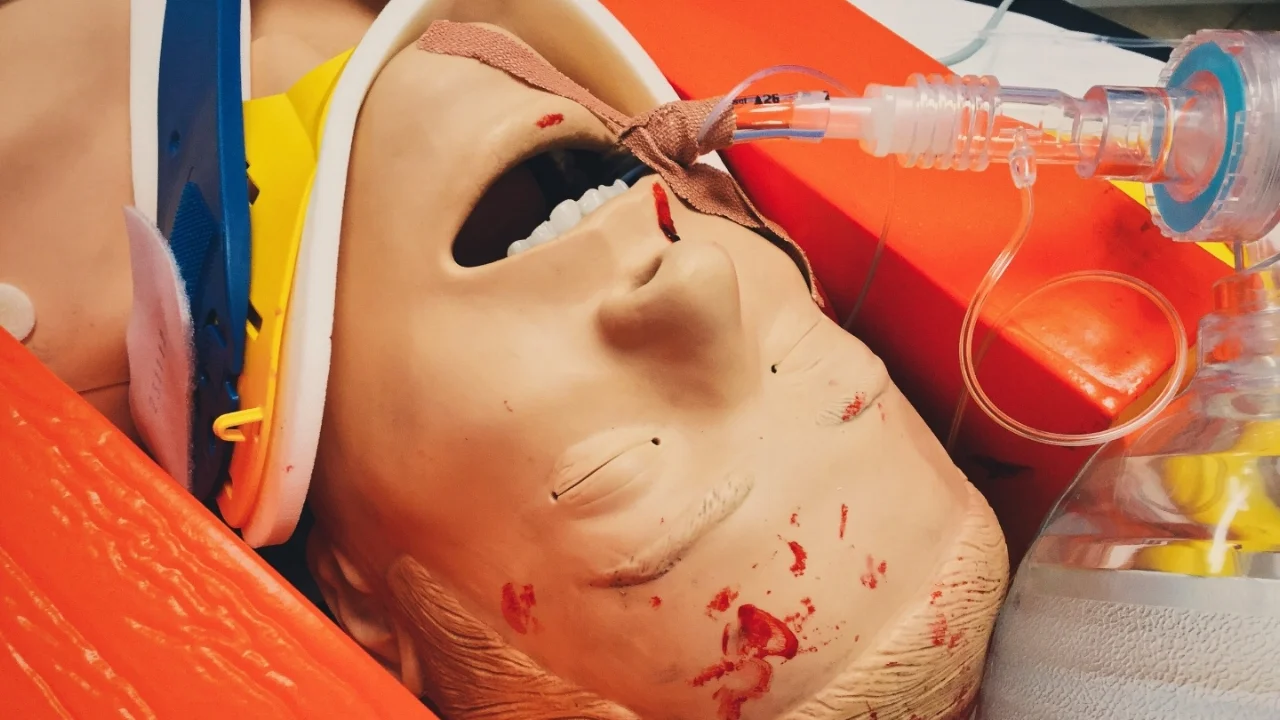
Head Injury
Why? How? When? Are they on anticoagulation? Consider and know the CT Head NICE Guidance (see below).
When examining head injuries in patients always check…
Eyes and CNs
Ears – haemotympanum?
Have a good feel at the lumps and bumps → if boggy, large or unsure get a senior to have a feel.
Any evidence of seizure? Wet themselves or bitten their tongue?
Resources
- NICE Guidance: Head Injury: Assessment and Early Management
- The Resus Room: Head Injury – Roadside to Resus & Devastating Brain Injury (podcasts)
Palliative Care
““Compassion. Compassion. Compassion!””
CPR is not a treatment for #ordinarydying. Every instance of futile CPR - which is what will happen if nobody has sorted out the protection of a DNACPR for someone whose life is coming to an end - is a tragedy. Please, doctors, nurses, patients, families - #havetheconversation. pic.twitter.com/t7yp6qm8Jd
— Linda Dykes (@DrLindaDykes) February 11, 2018
With too many health care professionals (and families) ducking #havetheconversation because it’s “too difficult” (actually, it usually isn’t) we need to empower individuals to demand the protection of a DNACPR. pic.twitter.com/8ShSXcjOni
— Linda Dykes (@DrLindaDykes) July 21, 2018
Resources
- St. Emlyns: Have a bit of ReSPECT for End of Life care
- RCEM Learning: Palliative Care in the ED
- Emergency Medicine Cases: End of Life Care in Emergency Medicine (podcast)