#SimBlog: Simple Case, Complex Environment
““15 year fell off his chair during his maths exam. Reduced responsiveness ‘slurring his words’ when lying on the floor ?may have taken something.””
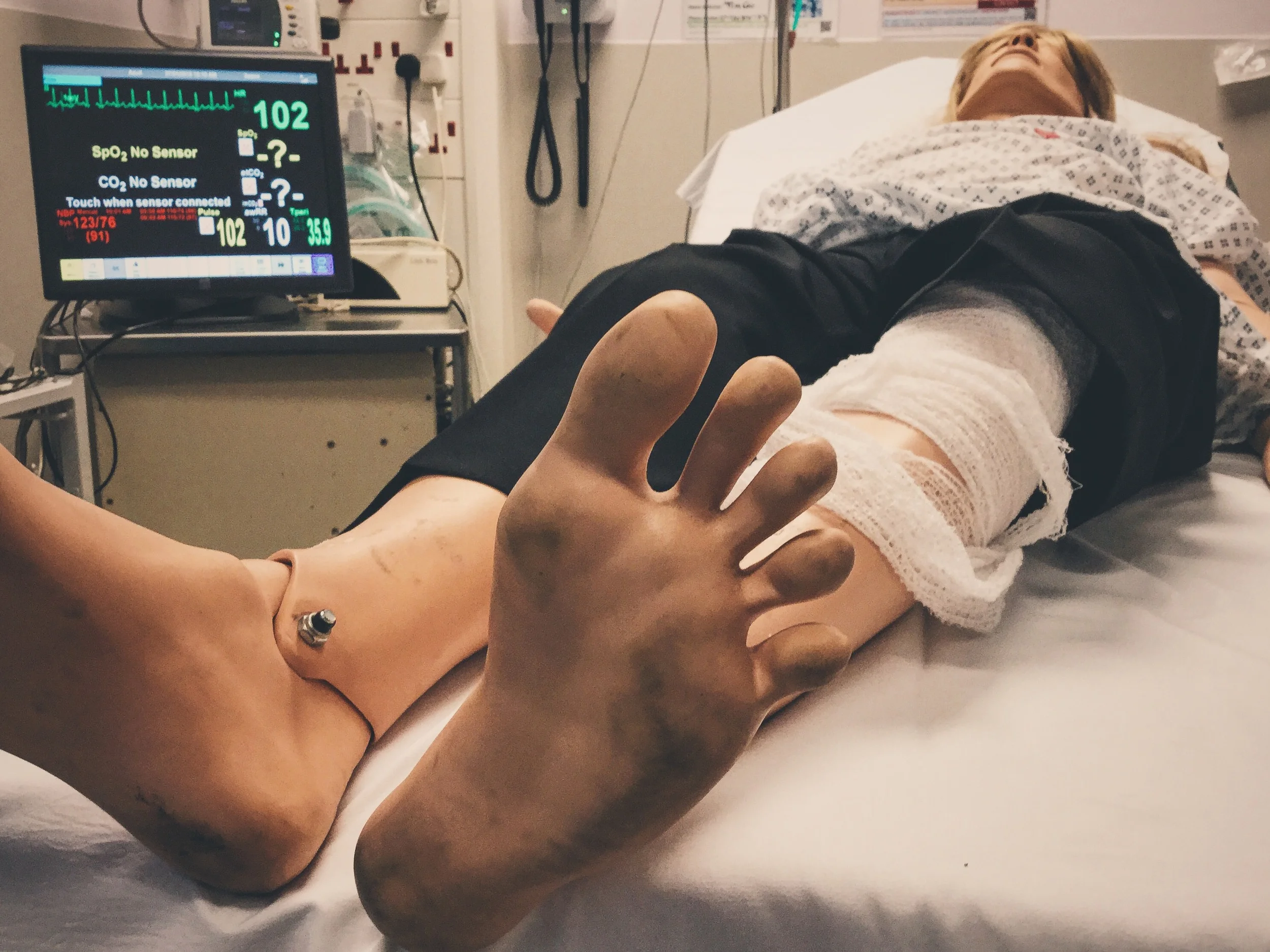
Observations
A – Patent
B – RR 16, Sats 99%
C – HR SR 80, CRT 2 sec, BP 120/80
D – V on AVPU
E – Temp 37°C
Clinical Findings
BM 2.0 (but this is not recorded or handed over on arrival)
Why We Simulated?
Working the ED can often be complicated, there can be distractions and developments that make even a simple case more complex than it should be.
In this case Karl is a 15 year old who has collapsed at school (he took his insulin but skipped breakfast and his blood sugar has fallen).
However several confounding factors were thrown in to make it a challenge.
Cannulation attempts are unsuccessful.
The WETFLAG sheet provided is for a 15 month old.
Distractions provided at the same time as the blood gas result.
This was all aimed at adding to the cognitive load on the clinician. Even if you have never heard of cognitive load you will have felt it when working in the ED. There is an excellent summary at EMDOCs.
Essentially your brain can only hold/process so much at any one time. Each distraction or decision you encounter takes up some cognitive load. Exceed what your brain can process and you may end up missing something.
How do we counter this? We need to offload:
Use tools/guidelines to help prompt your management (even using them as a checklist to ensure you haven't missed anything can help).
Understand you are limited – ask for help.
Handover/delegate tasks or patients if there is too much incoming.
Avoid interruptions (see point 3).
Use your team – bounce ideas or check if there is anything else they can think of.
Try to complete tasks before moving on.
Further Reading:
- EMDOCs: Cognitive Load and the Emergency Physician
- St. Emlyn's: Cliffhangers in the ED
Learning Outcomes
Can be beneficial to step back and summarise to keep the whole team informed.
Take time to look at and process results handed to you – step back or delegate the task. It takes cognitive load and if you have none to spare you may miss an abnormal result.
Remember alternative sources of information, previous attendances can give useful clues.
Positive Feedback
Team recognised abnormal BM
Identified alternative routes for administering treatment in the absence of IV access.
Compensated for distractions added through scenario – such as incorrect WETFLAG, interruptions, etc.