#SimBlog: Paediatric Trauma
The Scenario
“Paediatric Trauma Call (5 mins): Multi-vehicle road traffic accident with side-on collision. 8-year-old in rear passenger seat. C-spine immobilised, pain identified in left chest, left lower abdomen and left hip.”
Worse yet, there were next to no available staff for simulation. Thanks then to the medical students, allied health professionals and international clinical fellow all led by our resident PEM registrar. Of course, in reality a trauma team would gather, but forgiving this lack of fidelity our team stepped up and quickly identified the following during the primary survey…
<C> No sign of catastrophic haemorrhage
A: C-spine immobilised, talking full sentences
B: Trachea central, air entry bilaterally, some tenderness to left lower chest wall, no flail chest, no pneumothorax, no haemothorax, 15 breaths per minute, saturations 98%
C: HR 100 beats per minute, blood pressure 100/70mmHg, CRT 2 seconds, no visible bleeding
D: GCS 15/15, PERL, no signs of head injury
E: Tender right hip, right abdomen, temperature 36.5°C, no life threatening limb injuries
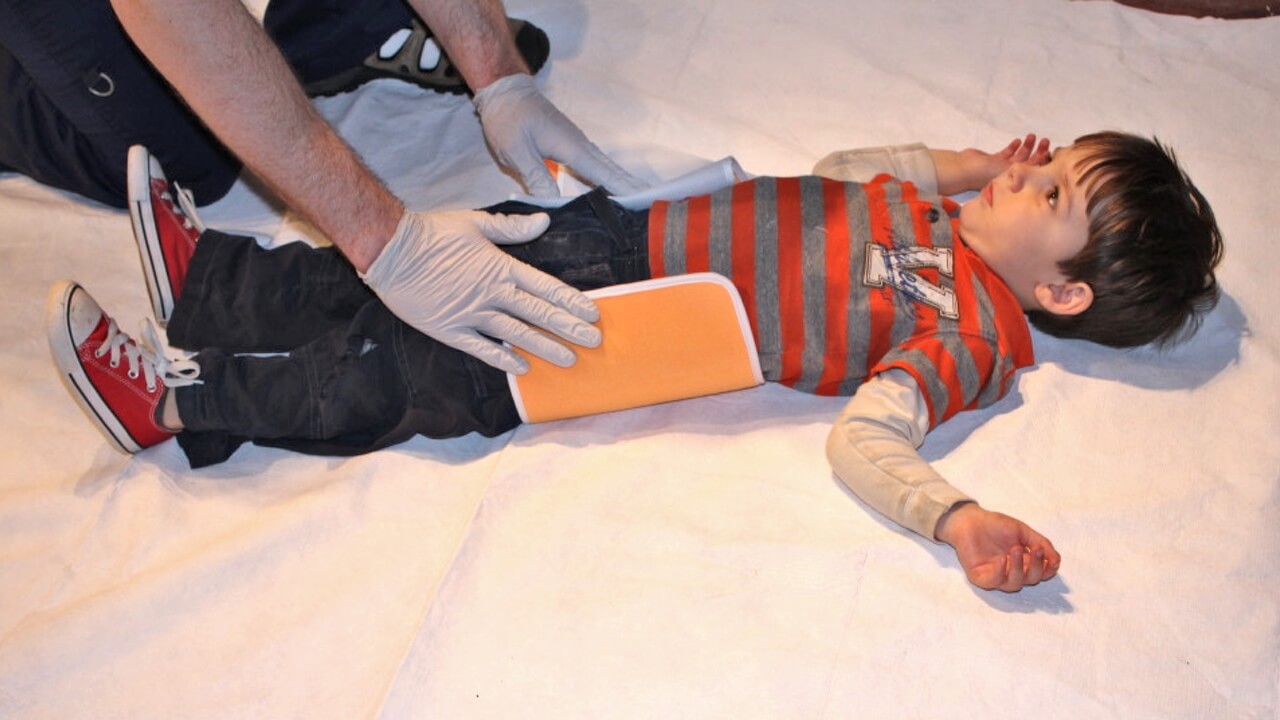
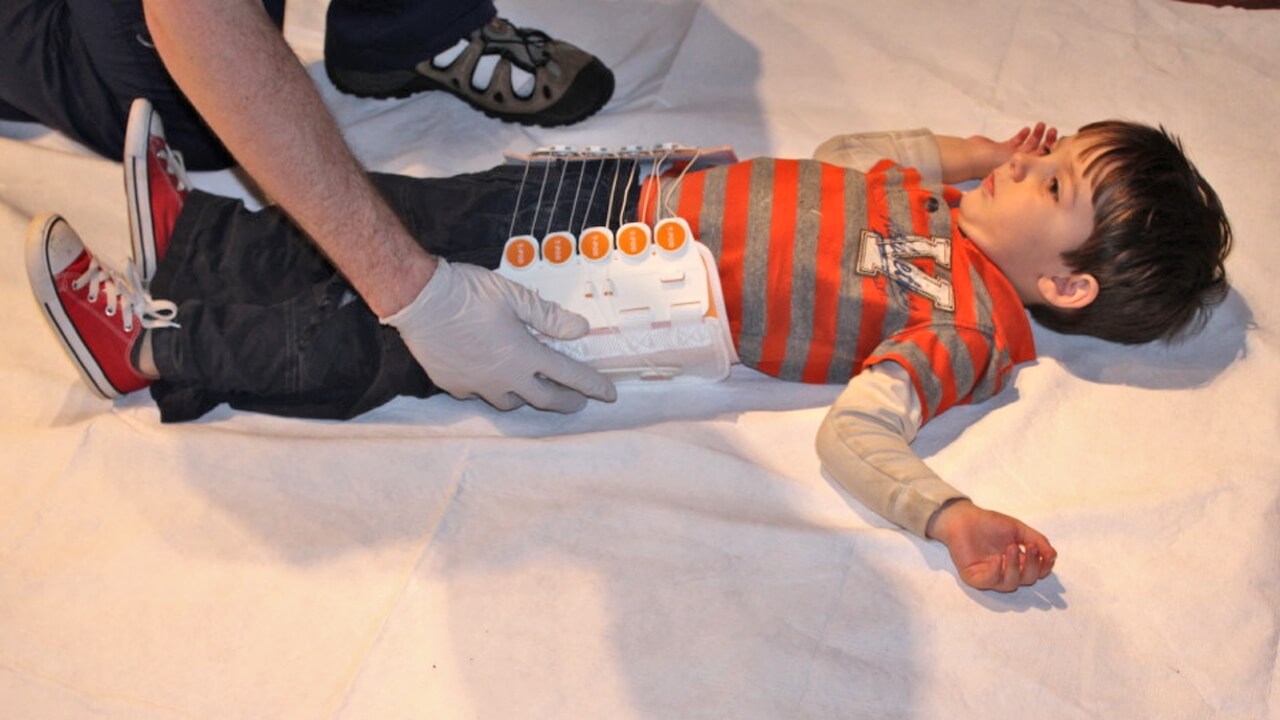
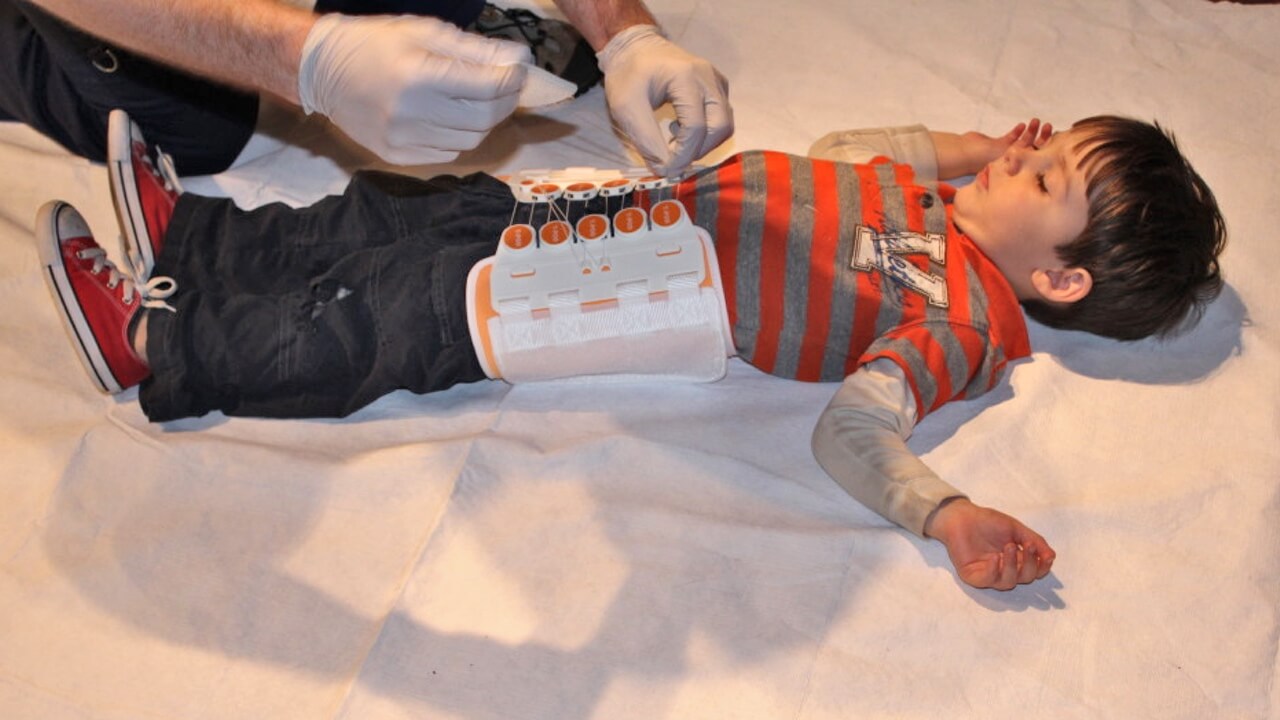
With the mother comforted and supported to calm the child, the pelvic binder was called for. Already adequate pain relief (intravenous morphine) was onboard and moments later the pelvic binder was in place and secured. Our child yelled out “get it off, get it off!”. It stayed on and efforts succeeded in reassuring and calming the child.
The Debrief
Following a short debrief focusing on the approach to paediatric trauma, we then took the opportunities to explore the use of the pelvic binder.
We then proceeded to discuss the Top 5 pelvic binder mistakes…
Examining with too much pressure
Log rolling more than 20 degrees
Not removing clothing first
Placing too high up in wrong position
Loosening the pelvic binder too early
So when do we need a pelvic binder?
Very simply, when we worry about pelvic fractures (see next section). Whilst their use has a largely evidence-free military history, they are widely regarded as effective and essential in protecting and securing the pelvis until definitive management follows.
Why do we worry about pelvic fractures?
Pelvic fractures can be life-threatening. When associated with major haemorrhage the bleeding can be difficult to identify let alone control. Pelvic fractures are less common in children as significant energy is required to fracture the paediatric pelvis. As such, other injuries commonly coexist alongside a paediatric pelvic fracture including, for example, significant abdominal or head injury. Bottom line: be vigilant.
So when would we suspect a pelvic fracture?
Well, as eluded to already, we would require a significant mechanism of injury such as a road traffic accident or fall from a significant height. In our case, we have some reason to be optimistic as lateral impacts are less concerning than anterior to posterior impacts. None the less, in this case we have good cause for concern, two vehicles colliding at speed mean all bets are off. Pelvic binders are not always applied prehospital. When they are in place on arrival in hospital it is important to (1) not to assume they are placed correctly and (2) not to remove them prematurely. It can be argued that if the mechanism is concerning, there is any cardiovascular instability or any reduced level in conscious level a pelvic binder should be applied and not removed until imaging can exclude significant fracture.
What about examination?
In short, be gentle as you could easily dislodge the “first clot” or worse still displace the fracture further. LOOK for bruising, asymmetry or deformity. FEEL bony landmarks (gently) including the iliac crests, posterior sacroiliac joints, ischial tuberosity and the spine. Include gentle COMPRESSION of the iliac crests. If pain or instability is identified, apply a pelvic binder and proceed to imaging.
What else?
Given the adjacent viscera, external genitalia and the urinary meatus should be examined for signs of bleeding. A perineal haematoma may elude to concealed bleeding also. Check the abdomen and consider lower limb symmetry, fractures and neurovascular status. Whilst not commonly performed in children rectal and vaginal examination may or may not be necessary.
So, pelvic XR or CT?
A pelvic x-ray is pragmatically available during ongoing resuscitation. As such, if “there is acute concern due to haemodynamic instability or uncertainty due to reduced conscious level or a distracting injury” then pelvic XR is a sensible choice (especially in children).
The exception to this is if CT imaging is planned for the abdomen acutely. In this case it is preferable to do away with pelvic XRs and proceed straight to CT.
Whatever the case or the role – the limitations of each modality must be understood. The pelvic XR is helpful at excluding a pelvic fracture as the causing of major haemorrhage, it cannot exclude pelvic fracture entirely.
Equally the role for CT pelvis is to determine definitively if there is a pelvic ring injury, however minor. It also characterises any such injury and informs management whereby interventional radiology may be suitable for addressing ongoing haemorrhage. Indeed, even when plain x-rays identify an injury, CT is often necessary at a later stage to delineate the detail of injury further and exclude associated injuries (both bony and visceral).