PEST Case 2: Using Your Team
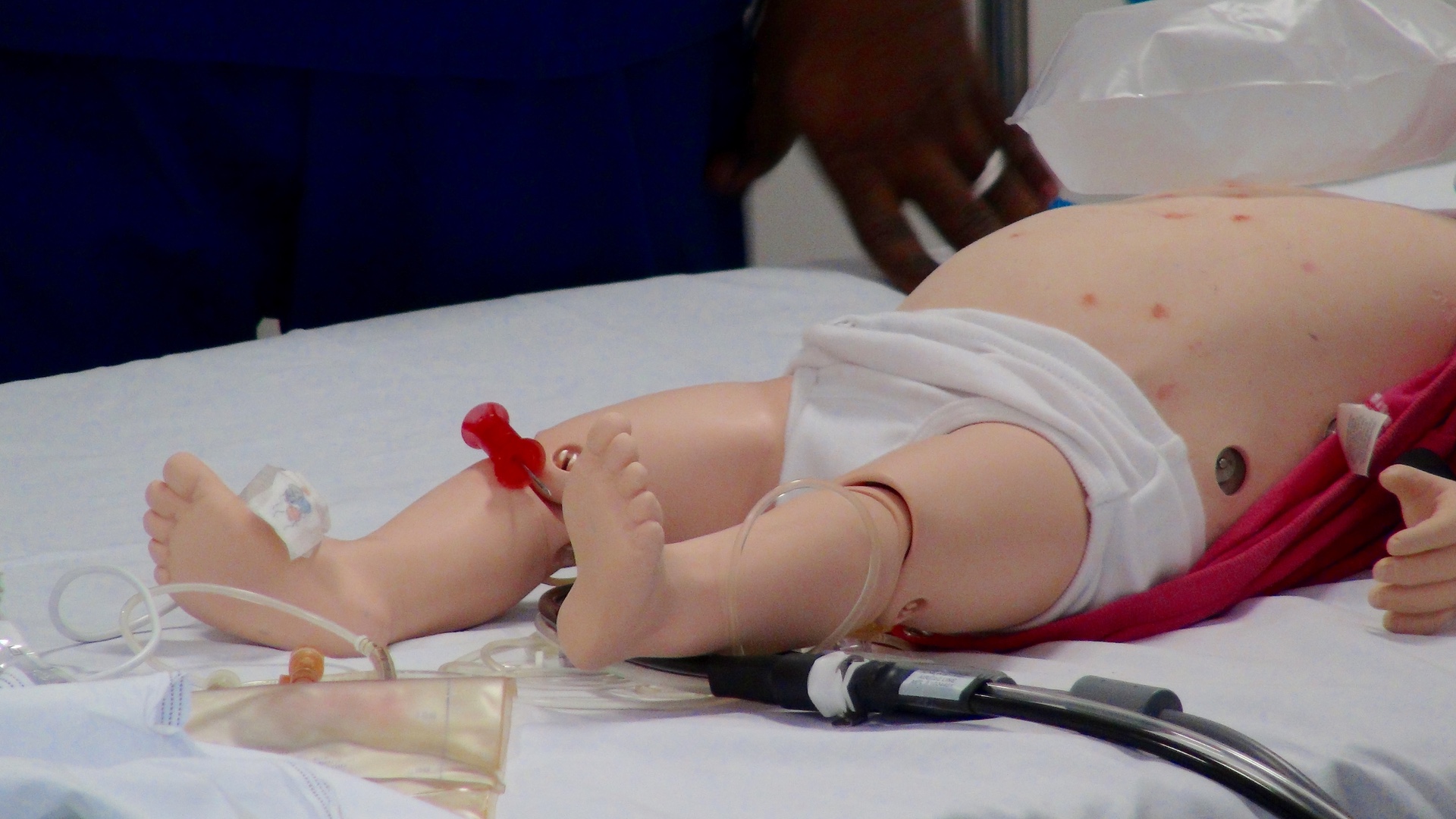
““A 9-month-old child arrives in Resus, he is drowsy with a temperature of 39°C.””
Assessment
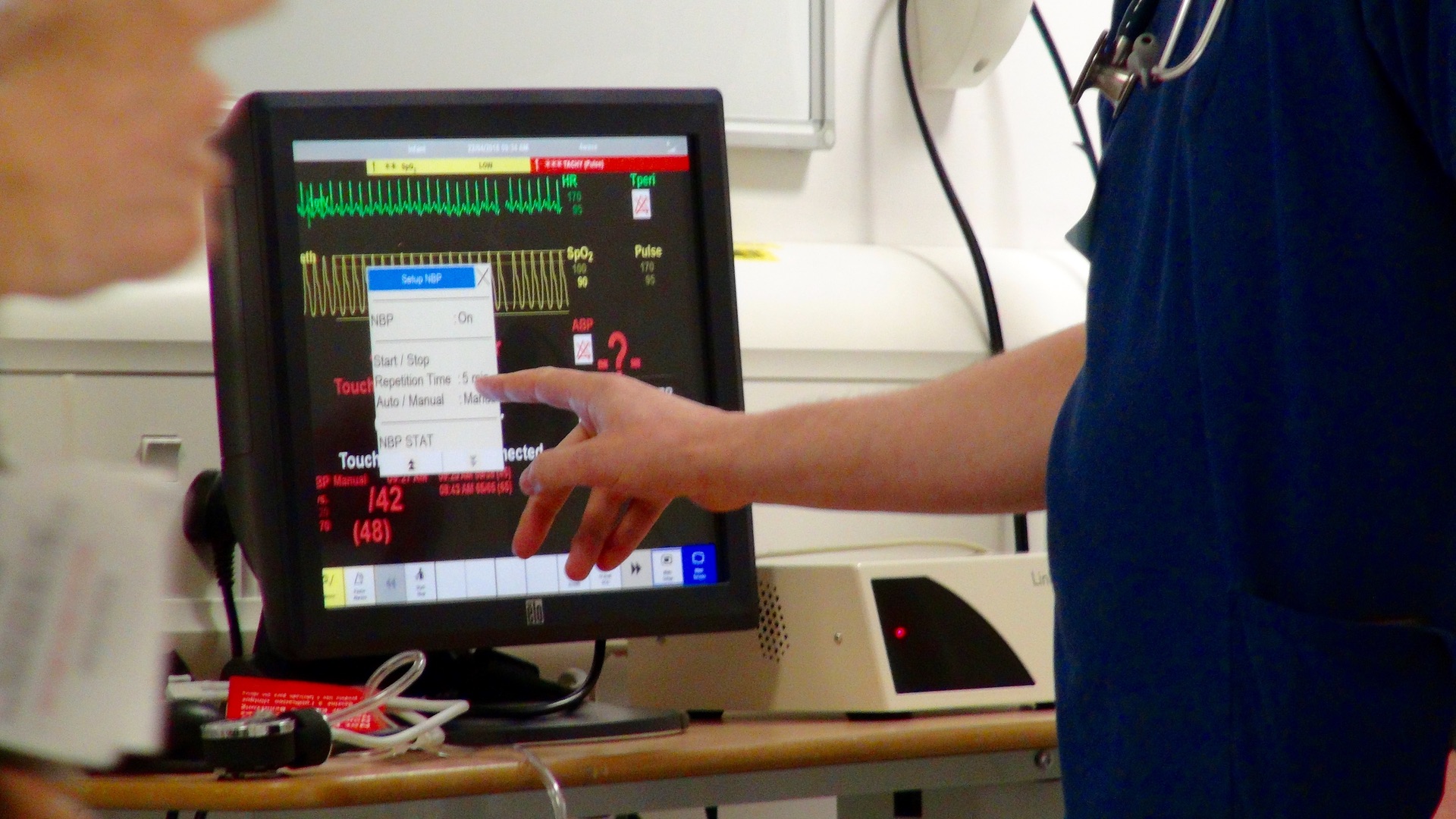
Clinical signs of shock with a non blanching purpuric rash.
Utilising your team…
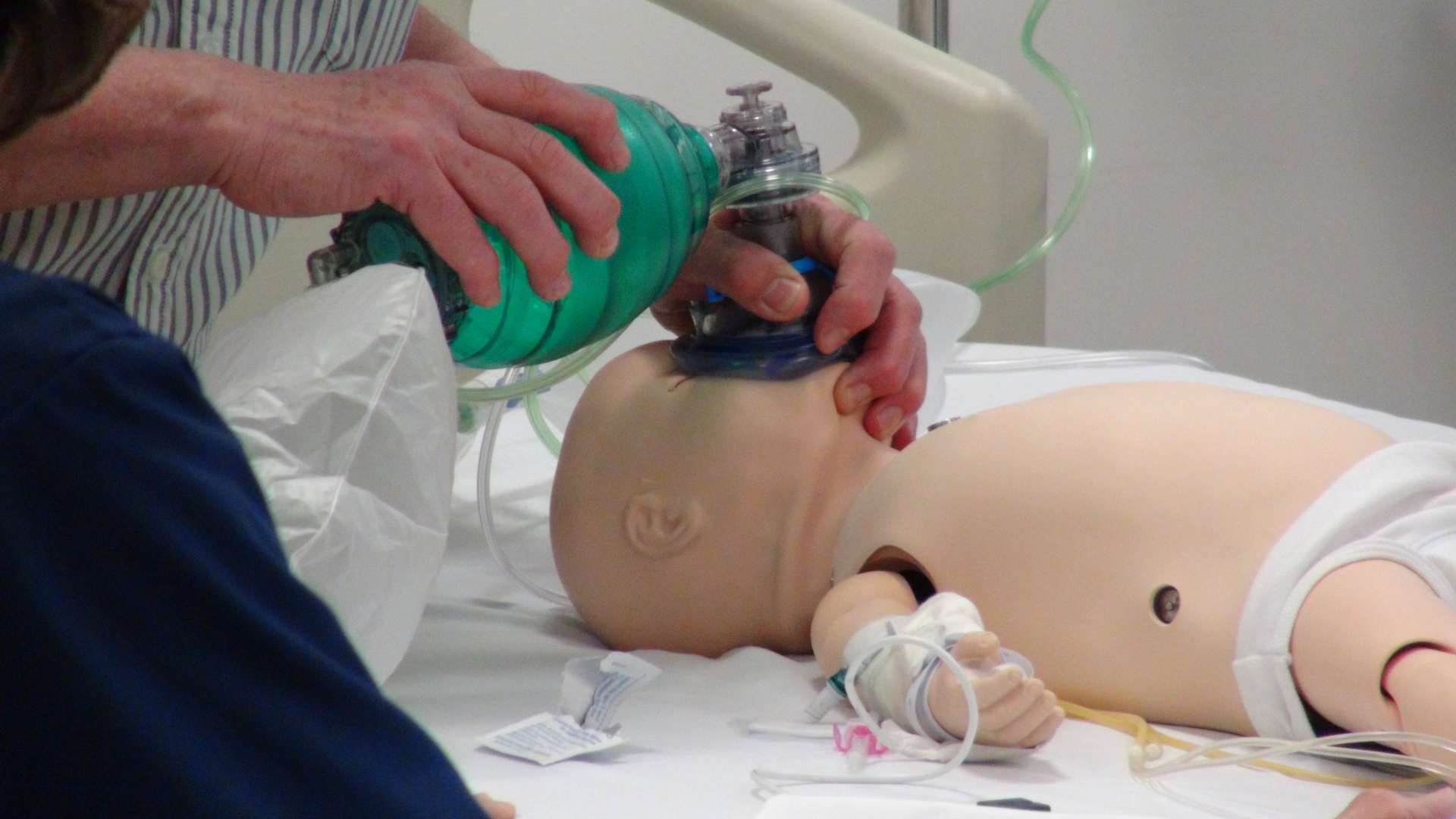
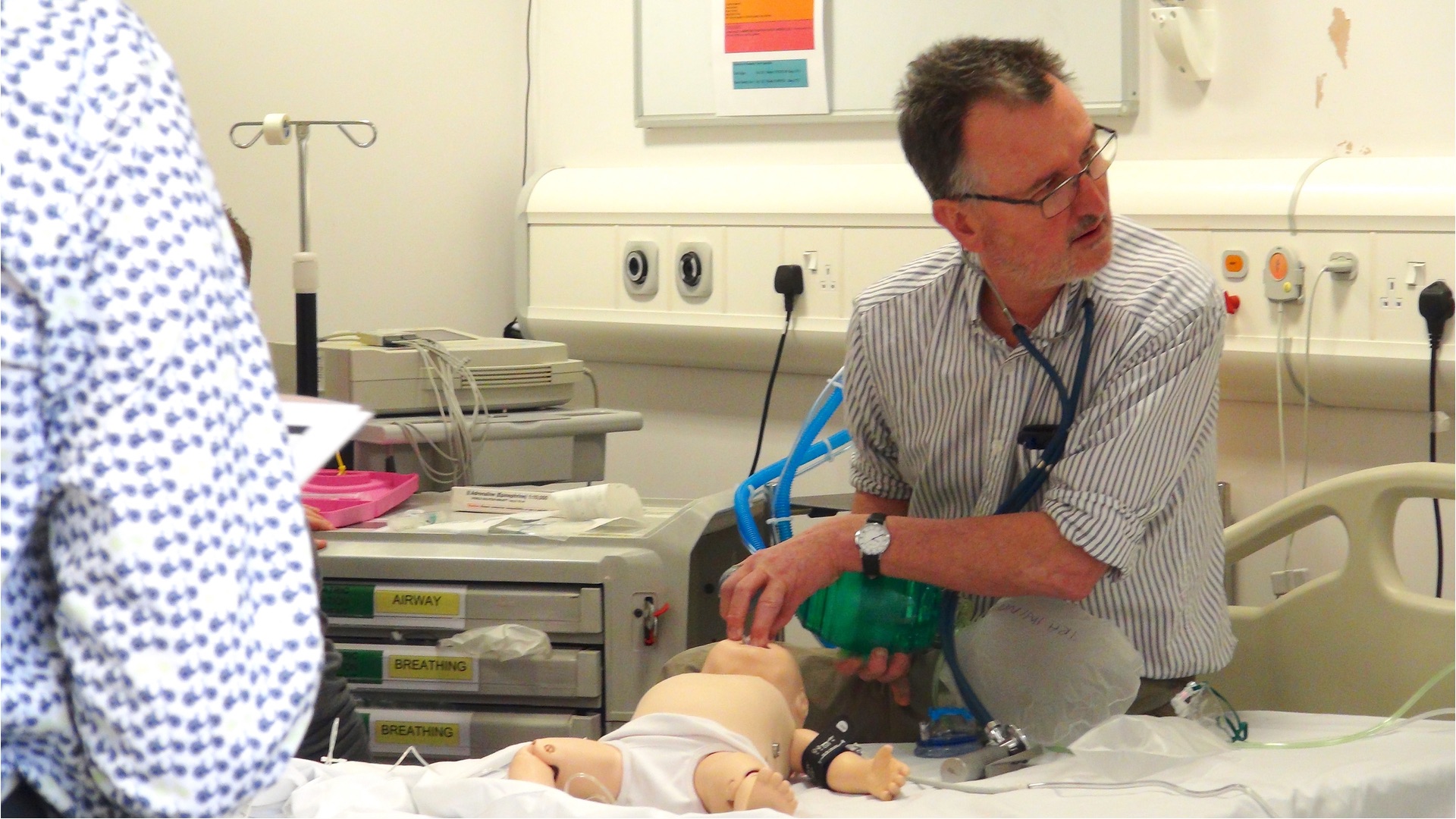
Scenarios based in the resuscitation room, particularly those where a ‘Red Call’ has been made, are often busy situations with plenty of personnel.
During the debrief, we discussed ways of maintaining situational control by utilising your team appropriately and how to create ‘space to think’ during difficult situations.
An often cited reason why you can’t compare medicine and aviation is the fact it is much easier to keep situational control in the peaceful cockpit of an aircraft. However we should still aim for the resuscitation room to be as organised an environment as possible.
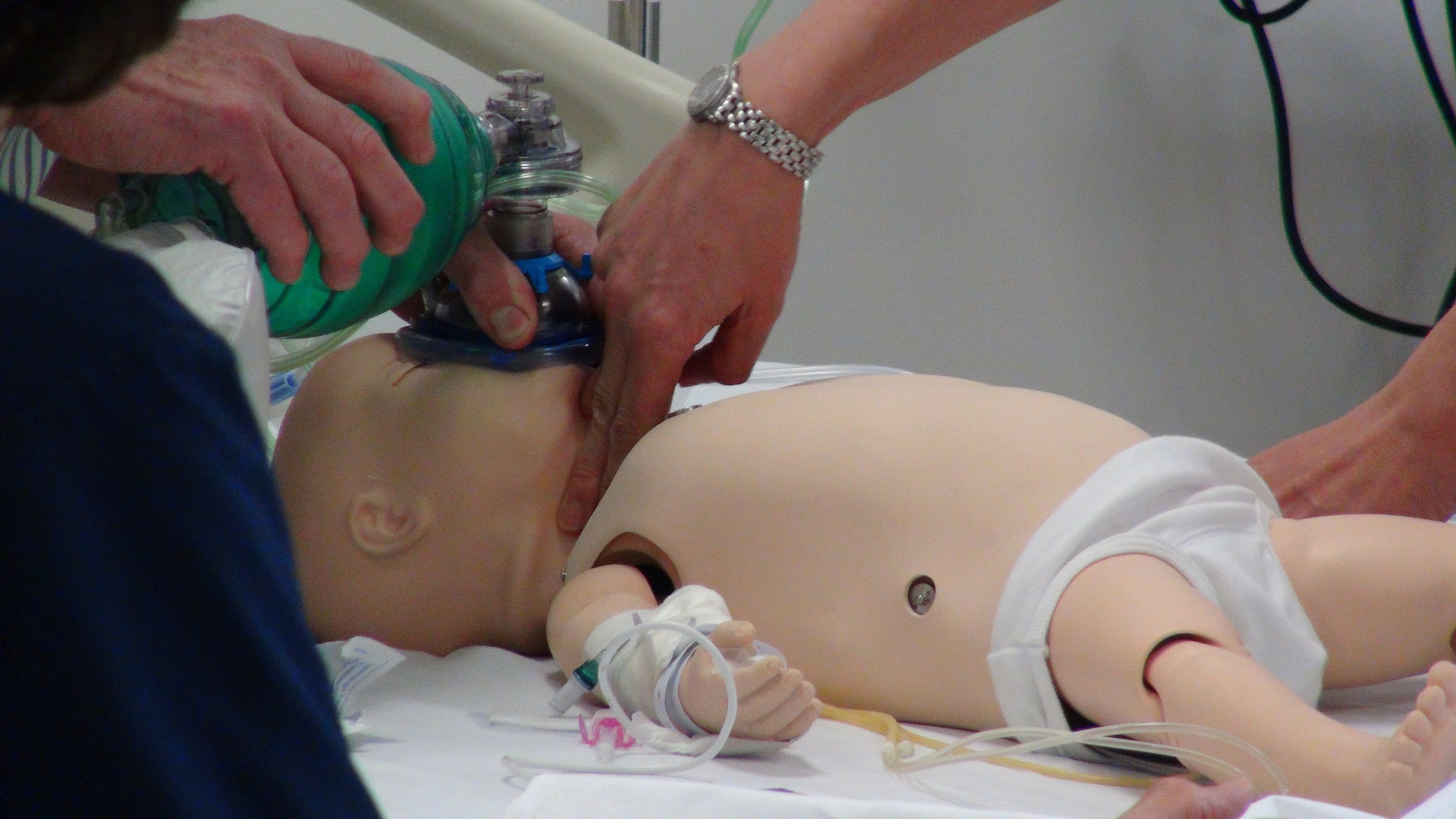
During this scenario, the team prepared for patient arrival by introducing themselves clearly, allowing the team leader to allocate roles appropriately. A rapid and structured A to E assessment was performed, which identified the risk of airway compromise, the need for urgent fluid resuscitation and antibiotic administration. IV access was not possible and there was closed loop discussion (link to Damian Roland’s blog) regarding this. There was rapid feed back to the team leader who recommended IO access, nominating a team member who was able to do this.
The child continued to deteriorate and the anaesthetic team recommended intubation. This proved difficult and the patient then deteriorated further with cardiac arrest. During the debrief, we discussed the decision to intubate and whether the team had a clear team appreciation of the potential risks of intubation. Planning for the ‘worst case scenario’ should this occur.
The Paediatric Intensive Care Consultant arrived during the cardiac arrest and asked the team leader ‘Do you want me to run the arrest?’. During the debrief we explored the offer as a potential opportunity to allow the team leader, who has a good knowledge of the case, space to think and consider further management.