Breathing Difficulty [Case #2]
“You are the senior doctor in Resus on a night shift when a mother brings in her 3 day old baby stating that he is appears blue and is not well.”
He had an uncomplicated delivery at term and was discharged home on the same day. Mum states that he had been feeding well initially but over the last 1 day he seems to have difficulty in breathing especially when he tries to breastfeed. This evening mum noticed a blue tinge to his lips and became concerned.
On examination he looks pale and centrally cyanosis is present. He is tachypnoeic at 70 bpm and has obvious chest wall retractions. Oxygen saturations on air were reported as 68% and on high flow oxygen were 75%. Chest auscultation reveals fine crackles throughout the lung fields but no heart murmurs. The blood pressure in the right arm and ankle were 60/45 mmHg.
QUESTIONS
Answer one question before attending the face-to-face teaching session. Add comments to answers already given if you think it's appropriate. The first part of teaching will be spent discussing this case:
- What will your initial management for this patient be?
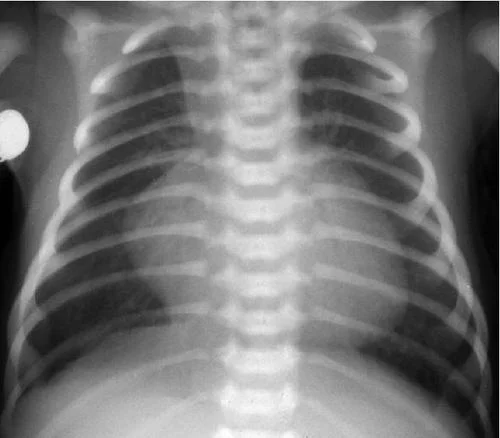
This is his CXR taken in Resus:
- What are the CXR findings?
- What is you differential diagnosis and what is the most likely cause of this presentation?
- How can you differentiate between a cardiac or respiratory cause for cyanosis in the neonate?
- What treatments can be started in Resus for this patient and explain their mechanism of action?


![Breathing Difficulty [Case #2]](https://images.squarespace-cdn.com/content/v1/546e1217e4b093626abfbae7/1470064591788-2JMPLP2V75CXV0JQOOKF/purple-banner.png)
![Pain, Minors & Painful Limbs [Case #1]](https://images.squarespace-cdn.com/content/v1/546e1217e4b093626abfbae7/1470065501632-LNF7DVFIMDSQQTDNML9W/blue-banner.png)
![Breathing Difficulty [Case #1]](https://images.squarespace-cdn.com/content/v1/546e1217e4b093626abfbae7/1470063857017-N0G366YDX4HM6XPXZLX3/purple-banner.png)