#MiniTeach: Another Paediatric Limp
It's 10:00pm on a Saturday night and a mother has brought in her 2-year-old son to children’s ED.
She has stated that he has been crying intermittently since the morning and mum has noticed that he isn’t walking normally on the right leg and thinks he may be in pain when attempting to walk.
She had given paracetamol at 3pm and was going to take him to see the GP in the morning but due to concern she brought him to ED tonight.
1. As the triage nurse what can you do for this child? What specific questions might you ask? What medication, if any, could you offer?
You could initially try and assess the pain he is in using pain chart.
Weigh the patient and prescribe analgesia for him. Paracetamol 15mg/kg and/or loading dose ibuprofen 10mg/kg if no contradictions.
He requires a set of observations including temperature and heart rate.
You may consider sending him for x-rays if you are able to illicit any specific area of tenderness.
2. As the first doctor to see this child what specific question will you ask in your history to differentiate the cause of the symptoms?
There is a limping child protocol that you should follow. This is included in the further reading.
After taking a history and examining the patient you ascertain that Tom is quite an active child for a 2 year old. His temperature is 37.2 and his other observation are unremarkable too.
When you go to see him he is stripped down to his nappy and playing happily with toys whilst sitting on a trolley. He has had no recent illnesses.
When mum attempts to stand him up Tom keeps his left up off the floor and when encouraged to place it down he starts to cry a little.
He is able to crawl on the trolley with no obvious discomfort.
On examining his leg he has no obvious swelling, bruising or deformity.
He appears to be moving his hip, knee and ankle normally both actively and passively.
It is unclear if he has any specific tenderness as he winces whenever you squeeze his leg.
3. What is the differential diagnosis?
In 0-4yr old consider:
Developmental: Hip dysplasia
Trauma: Toddler’s fracture/ Physeal fracture/ Puncture wound/ Sprain/ Contusion
Infectious: Osteomyelitis/ Septic arthritis/ Synovitis/ Discitis
Neoplasia: Various
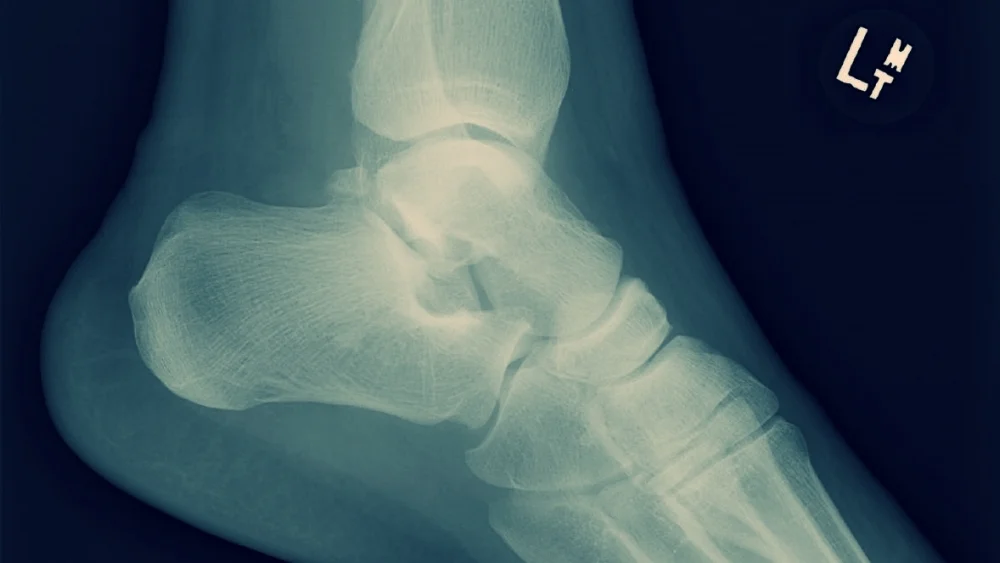
4. Describe the X-rays findings?
There is an undisplaced, incomplete spiral fracture to the distal third of the left tibia.
5. What specific questions might you ask if you are concerned about NAI? Is your concern justified?
Obtain a detailed history from the mother of what happened.
When it happened?
Who was witness to the events?
Who was caring for the child at that time?
Was anyone else around and who else has access to the child?
Any other siblings?
Is there a history of previous injuries and attendances to ED?
Are there any other signs or NAI?
Is the patient or siblings known to social services?
Concerns are probably not justified in this case as this is a Toddler’s fracture which can be a spiral fracture of the distal portion of the tibia and often results from minor trauma in ambulatory toddlers.
6. How would you treat this child? Where should he be followed up?
He will need an above knee cast and follow up in fracture clinic.
7. What advise would you give the parents?
Explain to the parents that this is a common fracture in this age group and they heal well with little complications when kept in a cast.
8. What is a CAST fracture? How is this different from a Toddler's fracture?
Ok so this was a little bit mean... A toddler’s fracture is also known as a “Childhood Accidental Spiral Tibial (CAST)” fracture. They are the same thing. In a Toddler’s fracture:
Fracture is not displaced.
Spiral or oblique pattern.
Involves distal half to distal third of the tibia.
Fractures of the more proximal tibia may be suspicious for non-accidental trauma.
Often as a result of minor mechanism, many times with a rotational component.
Initial x-rays commonly do not show evidence of Toddler’s Fracture (13-43%).
While there is no evidence in the literature to suggest that casting speeds healing, it does decrease the risk of displacement.
Useful Links:
http://pedemmorsels.com/toddlers-fracture/